Obesity is a widespread health issue that affects millions of people globally, with its consequences reaching far beyond just excess weight.
One of the less obvious but highly dangerous effects of obesity is lipid imbalance.
This imbalance, especially when left unchecked, can fuel a cascade of health problems, including heart disease, diabetes, and stroke.
But what exactly is the link between obesity and lipid imbalance, and how serious is it?
In this article, leanandfit.info shall explore the intricate relationship between obesity and lipid disorders, commonly referred to as dyslipidemia.
We shall reveal the alarming connection between excess body fat, high cholesterol, and the increased risk of life-threatening conditions.
Article Index:
- What is Lipid Imbalance?
- How Obesity Causes Lipid Imbalance
- High Cholesterol and Obesity: The Perfect Storm
- Overweight and Cholesterol: A Dangerous Combination
- How to Manage Lipid Imbalance in Obesity
- FAQs on Lipid Profile and Obesity
- The Shocking Conclusion: Is Obesity Fueling Lipid Imbalance?
What is Lipid Imbalance?
A lipid imbalance occurs when the levels of fats (lipids) in your blood are either too high or too low.
Lipids, which include cholesterol and triglycerides, are essential for building cells, storing energy, and producing certain hormones. However, when these lipid levels become unbalanced, they can lead to serious health problems.
For instance, high levels of low-density lipoprotein (LDL) cholesterol, often dubbed “bad cholesterol,” can contribute to the build-up of plaques in arteries, increasing the risk of cardiovascular diseases.
On the other hand, high-density lipoprotein (HDL) cholesterol, or “good cholesterol,” helps remove excess cholesterol from the blood.
In people who are obese, this balance between LDL and HDL often skews in the wrong direction, leading to what’s known as dyslipidemia—a condition characterized by abnormal lipid levels in the blood.
According to research from the American Journal of Clinical Nutrition, dyslipidemia is one of the most common complications associated with obesity, underscoring the dangerous relationship between weight gain and lipid health.
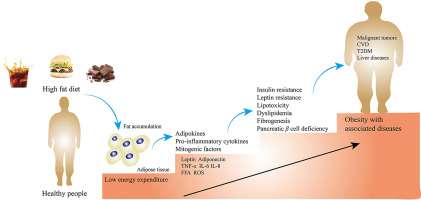
How Obesity Causes Lipid Imbalance?
Obesity has a direct influence on lipid metabolism, contributing to a lipid imbalance in various ways. When a person is obese, excess body fat, particularly around the abdominal area, triggers an inflammatory response in the body.
This inflammation alters the way fats are processed, leading to an increase in LDL cholesterol and triglycerides while decreasing HDL cholesterol.
This combination sets the stage for a dangerous cycle: fat tissue in obese individuals becomes more metabolically active, constantly releasing fatty acids into the bloodstream.
These excess fatty acids lead to elevated triglyceride levels and prompt the liver to produce more LDL cholesterol.
Meanwhile, HDL levels, which are responsible for clearing cholesterol from the blood, drop, making it harder for the body to maintain a healthy lipid profile.
A study published in The Lancet highlighted that obesity causes lipid imbalance by disrupting how the body regulates cholesterol and fat storage, further complicating the health risks associated with excess weight.
High Cholesterol and Obesity: The Perfect Storm
High cholesterol and obesity are closely linked, and together, they form a perfect storm for cardiovascular disease.
Obesity not only increases LDL cholesterol but also raises the levels of very low-density lipoproteins (VLDL), which are rich in triglycerides. This leads to a combination of high cholesterol and high triglycerides—one of the worst-case scenarios for heart health.
According to the World Health Organization (WHO), individuals who are obese have a significantly higher chance of developing hypercholesterolemia (high cholesterol), which further increases the risk of heart disease as it leads to cardiac overload.
The WHO also emphasizes that managing body weight is critical to reducing the risk of cholesterol-related complications.
Obesity, therefore, does not just increase the number on the scale—it also increases the amount of fat circulating in your bloodstream, making high cholesterol obesity one of the deadliest duos for your heart.
Overweight and Cholesterol: A Dangerous Combination
Even if you are not classified as “obese,” being overweight can also negatively affect your cholesterol levels. Studies show that people who are overweight often experience a gradual decline in their HDL cholesterol levels while seeing an increase in LDL cholesterol.
The relationship between overweight and cholesterol is often underestimated, but the risks are still very real.
A study published in the Journal of the American Heart Association found that for every 10% increase in body weight, the risk of dyslipidemia increases by 12%.
This statistic is alarming, particularly for individuals who may not consider themselves “obese” but are carrying excess weight.
The fat around the abdomen, in particular, is metabolically active and directly influences how cholesterol is processed in the liver. This makes being overweight a major contributor to the risk of high cholesterol and lipid imbalances.
FAQs on Lipid Profile & Obesity:
Q-1: How common is obesity in the United States, and why does it matter for lipid health?
A-1: Obesity is incredibly common in the U.S., affecting roughly 4 out of 10 adults. That is not just a number—it is a metabolic red flag.
When body fat increases, especially around the abdomen, it begins to interfere with how your body processes fats (lipids). This disruption can lead to higher levels of LDL (bad cholesterol) and triglycerides, while lowering HDL (good cholesterol).
Why does this matter? Because this trio—high LDL, high triglycerides, and low HDL—is the perfect storm for heart disease. In fact, a large percentage of individuals with obesity also struggle with lipid imbalances, making cardiovascular issues more likely over time.
Think of obesity as the “silent engine” behind lipid problems. It does not just sit there—it actively alters your metabolism.
The more excess fat you carry, the harder your body works to manage cholesterol properly. That is why tackling obesity isn’t just about weight loss—it is about protecting your heart, arteries, and long-term health.
Q-2: What is a lipid imbalance, and how is it linked to obesity?
A-2: A lipid imbalance—also known as dyslipidemia—occurs when your blood has unhealthy levels of fats like cholesterol and triglycerides. Now here is where obesity enters the picture: excess body fat directly interferes with lipid metabolism.
In people with obesity, the body tends to produce more triglycerides and very low-density lipoproteins (VLDL). At the same time, it struggles to maintain healthy HDL levels. This imbalance leads to a buildup of harmful fats in the bloodstream.
Even more concerning, obesity often changes the type of LDL particles. Instead of larger, less harmful ones, the body produces smaller, denser LDL particles—which are more likely to clog arteries.
In simple terms, obesity does not just increase fat—it changes how your body handles fat. That’s why lipid imbalance is so commonly seen alongside weight gain. If left unchecked, this combination can quietly damage your cardiovascular system over time.
Q-3: Can belly fat specifically worsen cholesterol levels?
A-3: Absolutely—and this is where things get serious. Belly fat, also known as visceral fat, is far more dangerous than fat stored elsewhere in the body. It sits around your organs and actively releases inflammatory chemicals and hormones that disrupt lipid balance.
This type of fat is strongly linked to higher triglycerides and lower HDL levels. It also contributes to insulin resistance, which further worsens cholesterol profiles. In fact, people with larger waistlines often have more severe lipid abnormalities—even if their overall weight isn’t extremely high.
Think of visceral fat as “metabolically active.” It is not just sitting there—it’s constantly sending signals that push your body toward imbalance.
The takeaway?
If your waistline is expanding, your lipid profile is likely taking a hit too. That is why reducing belly fat is one of the most effective ways to improve cholesterol and overall metabolic health.
Q-4: What are the warning signs that obesity is affecting your lipid levels?
A-4: Here’s the tricky part—lipid imbalances often don’t come with obvious symptoms. That’s why they’re often called “silent.” However, there are subtle clues your body might give you:
- Persistent fatigue or low energy
- Weight gain, especially around the abdomen
- Shortness of breath during mild activity
- Elevated blood pressure
- Blood sugar fluctuations
In more advanced cases, you might notice visible signs like fatty deposits under the skin or around the eyes. But for most people, the only reliable way to detect a lipid imbalance is through a blood test.
If you’re living with obesity, it’s wise to assume your lipid levels may already be affected. Regular screening becomes essential—not optional. Catching the problem early can prevent long-term damage to your heart and arteries.
Q-5: Does obesity increase the risk of heart disease through lipid imbalance?
A-5: Yes—and significantly so. When obesity leads to lipid imbalance, it creates the ideal conditions for plaque buildup in your arteries, a process known as atherosclerosis.
This plaque narrows blood vessels, reducing blood flow and increasing the risk of heart attacks and strokes. Add inflammation and insulin resistance into the mix, and the risk multiplies.
In the U.S., heart disease remains the leading cause of death, and obesity-related lipid disorders are a major contributor. The combination of high triglycerides, low HDL, and abnormal LDL particles accelerates arterial damage over time.
The scary part? This process can begin years before any symptoms appear. That’s why managing weight and lipid levels early is crucial. It’s not just about preventing disease—it’s about preserving your quality of life.
Q-6: Can weight loss improve lipid imbalance caused by obesity?
A-6: The good news? Yes—weight loss can make a dramatic difference. Even a modest reduction of 5–10% of body weight can significantly improve lipid levels.
When you lose weight, your body becomes more efficient at processing fats. Triglyceride levels drop, HDL levels rise, and LDL particles become less harmful. Essentially, your metabolic system starts to reset.
What’s even better is that these improvements can happen relatively quickly. Within weeks of adopting healthier habits, many people begin to see positive changes in their blood tests.
The key is consistency. Crash diets won’t deliver lasting results, but sustainable changes—like balanced eating and regular activity—can transform your lipid profile over time.
So yes, weight loss isn’t just cosmetic—it is a powerful tool for restoring metabolic balance.
Q-7: What role does diet play in obesity-related lipid disorders?
A-7: Diet plays a starring role—no question about it. Foods high in saturated fats, trans fats, and refined sugars can worsen lipid imbalance, especially in individuals with obesity.
When you consume these foods regularly, your body produces more harmful cholesterol and triglycerides. At the same time, it suppresses HDL, the “good” cholesterol that helps clean your arteries.
On the flip side, a heart-healthy diet can work wonders. Think:
- Fiber-rich foods like oats and vegetables
- Healthy fats from nuts, seeds, and olive oil
- Lean proteins and whole grains
These foods help reduce LDL and triglycerides while boosting HDL levels.
The bottom line?
Your plate directly influences your lipid profile. Small, consistent dietary changes can lead to big improvements in both weight and cholesterol levels.
Q-8: Is metabolic syndrome linked to obesity and lipid imbalance?
A-8: Yes—and it’s more common than most people realize. Metabolic syndrome is a cluster of conditions that includes obesity, high blood pressure, high blood sugar, and lipid imbalance.
In the U.S., a significant portion of adults fall into this category, making it a major public health concern. Central obesity (belly fat) is often the driving force behind this syndrome.
When these conditions occur together, the risk of heart disease, stroke, and type 2 diabetes skyrockets. Lipid imbalance plays a central role here, acting as both a symptom and a contributor to the problem.
Think of metabolic syndrome as a domino effect—obesity tips the first domino, and the rest follow. Addressing weight early can help prevent this cascade and protect your long-term health.
Q-9: How does inflammation from obesity affect lipid metabolism?
A-9: Obesity triggers chronic, low-grade inflammation in the body. This isn’t the kind of inflammation you feel—it is happening quietly at the cellular level.
This inflammation interferes with how your body processes lipids. It increases triglyceride production, lowers HDL levels, and promotes the formation of harmful LDL particles.
Over time, this inflammatory state damages blood vessels and accelerates plaque buildup. It is like adding fuel to the fire of cardiovascular risk.
What makes this particularly dangerous is that inflammation and lipid imbalance feed off each other, creating a vicious cycle. Breaking that cycle requires addressing the root cause—excess body fat.
Q-10: What are the best ways to reverse lipid imbalance caused by obesity?
A-10: Reversing lipid imbalance isn’t about one magic fix—it is about a combination of smart lifestyle choices:
- Lose weight gradually: Even small reductions make a big difference
- Move more: Aim for at least 150 minutes of moderate activity weekly
- Eat smart: Focus on whole, nutrient-dense foods
- Limit processed foods: Cut back on sugar and unhealthy fats
- Manage stress: Chronic stress can worsen metabolic health
- Sleep well: Poor sleep disrupts lipid regulation
For some individuals, medication may also be necessary, especially if lifestyle changes aren’t enough.
The key is consistency, not perfection. Think of it as a long-term investment in your health. With the right approach, you can not only improve your lipid profile but also reduce your risk of serious diseases down the line.
How to Manage Lipid Imbalance in Obesity?
If you’re struggling with obesity and a lipid imbalance, the good news is that there are effective ways to manage this condition. The most important step is weight loss.
Research has shown that even a modest weight loss of 5-10% can significantly improve lipid profiles, lowering LDL cholesterol and triglycerides while boosting HDL cholesterol.
Here are some strategies to consider:
Dietary Changes:
A heart-healthy diet that includes plenty of fruits, vegetables, whole grains, and lean proteins can help lower cholesterol levels. The Mediterranean diet, in particular, has been shown to improve lipid profiles in individuals with obesity.
I lost several pounds in just a few months after including homemade Weight Loss Smoothies in my diet plan.
Physical Activity:
Regular exercise not only aids in weight loss but also directly improves lipid metabolism.
Aerobic exercises such as walking, planks for weight loss, swimming, and cycling are especially effective at lowering LDL cholesterol and raising HDL cholesterol.
Medications:
In some cases, cholesterol-lowering medications such as statins may be prescribed. These drugs help lower LDL cholesterol levels and are often recommended for individuals with both high cholesterol and obesity.
However, they should always be used in conjunction with lifestyle changes.
Monitoring and Testing:
Regular blood tests to monitor cholesterol levels and overall lipid health are essential for managing a lipid imbalance. Early detection of high cholesterol can help prevent the development of more serious conditions, such as heart disease or stroke.
According to a study in the Journal of Clinical Lipidology, losing weight through lifestyle changes or surgery has a profound impact on lipid levels.
In individuals who had weight-loss surgery, for example, LDL cholesterol levels dropped significantly within six months, underscoring the importance of weight management in controlling lipid disorders.
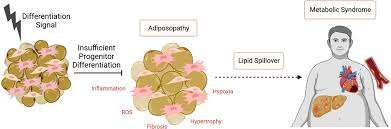
The Shocking Conclusion: Is Obesity Fueling Lipid Imbalance?
The short answer is a resounding yes—obesity causes lipid imbalance, and this imbalance can have severe consequences for your health.
The connection between high cholesterol and obesity is well-established, with excess body fat leading to increased levels of LDL cholesterol, triglycerides, and other harmful lipids. This imbalance raises the risk of heart disease, stroke, and even diabetes.
However, the good news is that addressing obesity through lifestyle changes—such as adopting a healthier diet, increasing physical activity with bodyweight workouts, and, if necessary, using medications—can help manage and even reverse lipid imbalances.
The earlier you take action, the better your chances of avoiding the long-term complications associated with high cholesterol and lipid disorders.
In conclusion, while obesity and high cholesterol obesity are dangerous, they do not have to be a life sentence. With the right approach, you can regain control of your health, balance your lipid levels, and reduce the risk of serious cardiovascular complications.
Take steps today to address the underlying causes of your lipid imbalance, and you will be on your way to a healthier, longer life.
References: