Obesity is often associated with common health risks like diabetes and joint problems, but what about its hidden impact on the heart?
Cardiac overload, a condition where the heart is overworked due to increased demands from the body, is one of the lesser-discussed consequences of obesity.
As your body size increases, so does the strain on your heart, leading to various complications that could become life-threatening if left unchecked.
In this article, leanandfit.info will explore how obesity contributes to cardiac overload, the signs and symptoms to watch for, and ways to address this issue before it spirals out of control.
Points Covered in this Article:
- What is Cardiac Overload?
- Cardiac Volume Overload and Obesity
- Pressure Overload in the Heart
- Cardiac Fluid Overload: Causes and Risks
- Signs of Cardiac Overload
- Cardiac Iron Overload and Obesity
- Can Cardiac Overload be Reversed?
- FAQs on Cardiac Overload and Obesity
- Conclusion: Is Cardiac Overload the Hidden Danger of Obesity?
What is Cardiac Overload?
Cardiac overload occurs when the heart is forced to work harder than normal to pump blood throughout the body.
This can happen in two forms: pressure overload and volume overload. In both cases, the heart becomes strained and may begin to enlarge or weaken over time.
Obesity, with its added body mass and increased metabolic demands, can lead to cardiac overload, placing significant stress on the cardiovascular system.
Scientific research published in The Journal of Clinical Investigation confirms that obesity is a major contributing factor to heart disease due to this overload mechanism.
Cardiac Volume Overload and Obesity
In the context of obesity, cardiac volume overload occurs when the heart is forced to manage an increased blood volume due to excess body fat.
As body fat increases, so does the body’s total blood volume, placing additional demand on the heart. Imagine your heart as a pump designed for a specific capacity—when the volume exceeds what it’s built for, it must work harder to keep up.
In someone with a healthier weight, this demand is manageable, but in individuals with obesity, the constant overwork can weaken heart muscles over time, increasing the risk of conditions like heart failure.
This risk is significantly higher when leptin resistance is also present.
Leptin, a hormone primarily involved in regulating appetite and metabolism, also affects cardiovascular health. When leptin signaling fails, it promotes chronic inflammation and further stresses the heart.
A study in The American Journal of Cardiology confirmed that obesity-induced cardiac volume overload directly accelerates heart disease, especially in individuals with high body mass index (BMI).
Persistent strain on the heart leads to left ventricular hypertrophy (enlargement of the heart’s main pumping chamber), which can result in arrhythmias and long-term heart failure if left unchecked.
Recognizing and managing cardiac volume overload early is crucial to preserving heart function.
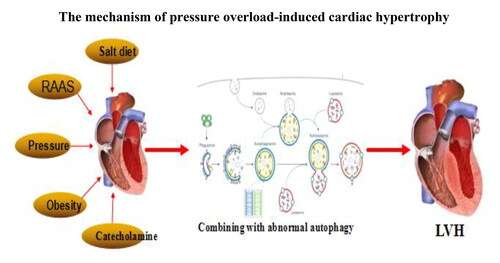
Pressure Overload in the Heart
Pressure overload in the heart is another type of strain associated with obesity. When blood pressure increases due to obesity, the heart has to pump against greater resistance in the arteries.
This type of overload makes the heart work harder to move blood, leading to thickening of the heart muscles, especially in the left ventricle.
Over time, this thickening can result in a loss of flexibility, making the heart less efficient at pumping blood. This increases Atherosclerosis Risk in Obesity.
According to the Journal of Hypertension, people who are obese are significantly more likely to experience pressure overload, leading to long-term cardiovascular complications.
Cardiac Fluid Overload: Causes and Risks
In some cases, obesity can lead to cardiac fluid overload, a condition where the body retains excess fluids.
When this happens, the heart has to pump not only an increased blood volume but also manage the additional fluid, which puts more strain on the heart.
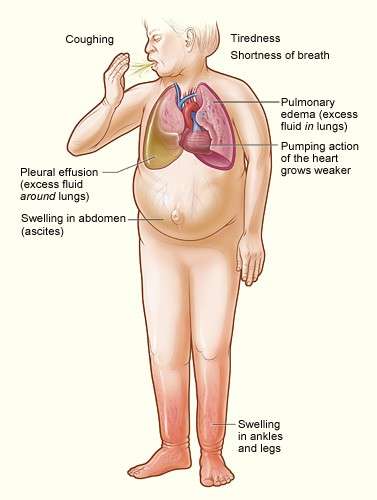
This often results in swelling (edema) in the legs, ankles, and abdomen. Cardiac fluid overload can be a precursor to congestive heart failure if not managed promptly.
Health professionals often use diagnostic codes like cardiac volume overload ICD-10 to classify and treat this condition. It has also been ascertained that obesity impacts your cardiovascular health.
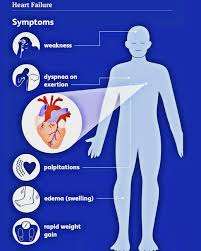
Signs of Cardiac Overload
Recognizing signs of cardiac overload is crucial for early intervention and preventing serious heart conditions.
Common symptoms include shortness of breath during physical activity or even at rest, persistent fatigue, chest pain or tightness, and swelling in the lower extremities, particularly the ankles and feet.
These signs indicate that the heart is struggling to pump blood efficiently, which can lead to fluid retention and increased pressure on the cardiovascular system.
If left untreated, cardiac overload can progress to heart failure or other life-threatening conditions.
For example, an individual with obesity may experience frequent shortness of breath and assume it’s due to poor fitness or weight alone, overlooking the possibility of an underlying cardiac problem.
According to the American Heart Association, early recognition of these symptoms can significantly improve outcomes, particularly for individuals with risk factors like hypertension, obesity, and diabetes.
Scientific studies, such as one published in Circulation, highlight that heart failure patients who receive treatment at the early stages of cardiac overload have a far better prognosis than those diagnosed at advanced stages.
Identifying warning signs early allows for interventions like lifestyle changes, medications, and improved blood pressure management, ultimately reducing the risk of long-term heart complications.
Cardiac Iron Overload and Obesity
Let’s talk about another sneaky culprit behind heart problems in obese individuals—cardiac iron overload.
Sounds fancy, but it is basically what happens when too much iron builds up in the heart tissue.
While your body needs iron to survive (hello, red blood cells), too much of it in the wrong place can spell trouble.
Excess iron can cause inflammation and damage in the heart, eventually leading to heart dysfunction or, worse, heart failure.
Now, you might think cardiac iron overload is something only people with genetic conditions like hemochromatosis need to worry about.
But here is the kicker—research suggests that individuals with obesity may experience altered iron metabolism, leading to increased iron deposition in the heart.
Essentially, the body’s iron-regulating system gets thrown out of whack, piling even more stress on an already overworked heart.
Think of it this way: obesity is like carrying an overpacked suitcase on a long journey, and cardiac iron overload is that extra unnecessary weight stuffed in at the last minute.
The result?
A heart that is tired and struggling to keep up.
Studies published in Cardiology Journal emphasize that addressing altered iron metabolism could be key to improving cardiac outcomes in people with obesity.
Can Cardiac Overload be Reversed?
The good news is that cardiac overload is not necessarily a one-way street.
Lifestyle changes, such as weight loss, increased physical activity, and improved dietary habits, can reduce the strain on the heart.
Medications to manage blood pressure, reduce fluid retention, and control cholesterol levels can also help.
In severe cases, medical interventions such as bariatric surgery may be considered to reduce obesity-related heart strain.
According to a study published in Circulation, weight loss significantly reduces the risk of developing heart failure, even in people who already have some degree of cardiac overload.
FAQs on Cardiac Overload and Obesity:
Q-1. How does obesity cause cardiac overload and heart strain?
A-1. Obesity forces your heart to work harder than normal, creating what is known as cardiac overload. As body weight increases, the body requires more oxygen and nutrients, which means the heart must pump more blood.
In the United States, where over 42% of adults are obese, this added demand is a widespread issue.
This leads to increased blood volume and cardiac output, placing constant stress on the heart—especially the left ventricle, which is responsible for pumping oxygenated blood throughout the body.
Over time, this strain causes the heart muscle to thicken and lose efficiency.
Think of it like running a machine nonstop at high capacity—it eventually wears down.
Cardiac overload is often silent at first, but it gradually weakens the heart, increasing the risk of long-term cardiovascular complications.
Q-2. What are the early signs of cardiac overload due to obesity?
A-2. Cardiac overload doesn’t usually show obvious symptoms in its early stages, which makes it dangerous. However, there are subtle warning signs to watch for:
- Shortness of breath during light activity
- Fatigue or reduced stamina
- Swelling in the legs or ankles
- Rapid or irregular heartbeat
- Difficulty lying flat without discomfort
In the U.S., millions of adults experience these symptoms but often attribute them to aging or low fitness levels. In reality, they can be early indicators of heart strain caused by excess weight.
Recognizing these signs early can make a big difference. Addressing obesity at this stage can help reduce cardiac stress and prevent more serious complications down the line.
Q-3. What is the link between obesity and left ventricular hypertrophy?
A-3. Left ventricular hypertrophy (LVH) is a condition where the heart’s main pumping chamber thickens due to increased workload. Obesity is a major contributor to this condition.
As the heart works harder to circulate blood through a larger body mass, the left ventricle adapts by becoming thicker and stronger initially. However, this adaptation eventually becomes harmful.
The thickened muscle becomes less flexible, reducing the heart’s ability to fill and pump efficiently.
In the U.S., LVH is increasingly common among individuals with obesity and high blood pressure. It’s considered a key step in the progression toward heart failure.
The important thing to understand is that while LVH starts as a compensatory response, it ultimately leads to decreased heart function if not addressed.
Q-4. Does excess body weight significantly increase heart workload?
A-4. Yes, excess body weight significantly increases heart workload. For every additional pound of body weight, the heart must pump blood through miles of blood vessels, increasing overall strain.
In obese individuals, total blood volume can increase by up to 30–50%, which directly raises the heart’s workload. This constant demand forces the heart to pump more frequently and with greater force.
In the U.S., where sedentary lifestyles are common, this added strain is often compounded by lack of physical activity, making the heart even less efficient over time.
The result is a cycle where increased weight leads to higher workload, which then reduces the heart’s ability to function effectively. Breaking this cycle is essential for maintaining cardiovascular health.
Q-5. What are the heart failure risks linked to obesity in U.S. adults?
A-5. Obesity is one of the leading risk factors for heart failure in the United States.
Studies show that individuals with obesity have a significantly higher likelihood of developing heart failure compared to those with a healthy weight.
Heart failure occurs when the heart can no longer pump blood effectively. In obese individuals, prolonged cardiac overload weakens the heart muscle, making it less efficient over time.
In the U.S., heart failure affects millions of adults, and a large proportion of these cases are linked to obesity-related conditions such as high blood pressure, diabetes, and lipid imbalance.
The risk increases with both the duration and severity of obesity, making early intervention critical.
Q-6. How does fat accumulation affect heart structure and function?
A-6. Fat accumulation doesn’t just affect appearance—it directly impacts heart structure and function. Excess fat, particularly visceral fat, releases hormones and inflammatory substances that alter how the heart works.
This can lead to structural changes such as enlargement of the heart chambers and thickening of the heart walls. Functionally, the heart becomes less efficient at pumping blood and maintaining proper circulation.
In the U.S., where abdominal obesity is common, these changes are frequently observed even in younger adults. Over time, this can lead to reduced cardiac output and increased risk of heart disease.
In simple terms, excess fat reshapes and weakens the heart, making it less capable of handling everyday demands.
Q-7. Can obesity lead to chronic cardiac overload symptoms?
A-7. Yes, obesity can lead to chronic cardiac overload, where the heart is under constant strain for extended periods.
This long-term stress eventually leads to noticeable symptoms such as persistent fatigue, shortness of breath, and reduced exercise tolerance.
In the U.S., many adults live with these symptoms without realizing they are related to heart strain.
Chronic overload can also contribute to fluid retention, leading to swelling in the lower limbs.
Over time, this condition can progress to more serious issues like heart failure.
The longer the heart remains under strain, the harder it becomes to reverse the damage.
That is why early lifestyle changes are essential to reduce the burden on the heart.
Q-8. How does obesity impact blood volume and cardiac output?
A-8. Obesity increases both blood volume and cardiac output, which directly contributes to cardiac overload.
As body mass increases, the circulatory system expands to supply oxygen and nutrients to additional tissue.
This means the heart must pump more blood with each beat. In some cases, cardiac output can increase by up to 20–30% in individuals with obesity.
In the U.S., this increased demand is a common underlying factor in obesity-related heart conditions.
While the heart initially adapts to this demand, prolonged stress eventually leads to reduced efficiency and function.
Managing body weight helps reduce this burden and allows the heart to operate more efficiently.
Q-9. Why does obesity increase the risk of arrhythmias and heart failure?
A-9. Obesity increases the risk of arrhythmias (irregular heartbeats) and heart failure due to structural and electrical changes in the heart.
Excess fat and inflammation can disrupt the heart’s normal rhythm, leading to conditions like atrial fibrillation.
In the U.S., atrial fibrillation affects millions of adults, and obesity is a major contributing factor.
Additionally, cardiac overload weakens the heart muscle, making it more prone to failure.
The combination of structural changes, inflammation, and increased workload creates an environment where both rhythm disorders and heart failure can divert simultaneously.
Maintaining a healthy weight helps reduce these risks and supports better heart function.
Q-10. How does long-term obesity damage the cardiovascular system?
A-10. Long-term obesity affects the entire cardiovascular system, not just the heart.
It leads to increased blood pressure, inflammation, and lipid imbalances, all of which damage blood vessels and reduce circulation efficiency.
In the U.S., cardiovascular disease remains the leading cause of death, and obesity is a major driver.
Over time, arteries become stiff and narrow, increasing the risk of heart attacks and strokes.
The heart, blood vessels, and metabolic systems are all interconnected, so prolonged obesity creates widespread damage.
The good news is that many of these effects can be improved or even reversed with consistent lifestyle changes.
Final Takeaway:
Cardiac overload is a hidden but serious consequence of obesity, affecting millions of adults across the United States.
While it often develops silently, its impact on heart structure, function, and overall health is significant.
The key to prevention lies in early awareness, consistent lifestyle changes, and maintaining a healthy weight.
By reducing the strain on your heart, you can protect your cardiovascular system and improve your long-term quality of life.
Conclusion
So, is cardiac overload the hidden danger of obesity?
Absolutely. While obesity has long been recognized for its role in contributing to diabetes, joint problems, and sleep apnea, its impact on the heart—particularly through cardiac overload—remains under-discussed.
Obesity places enormous stress on the heart, whether through cardiac volume overload, pressure overload in the heart, or even more specific issues like cardiac iron overload. I have shed countless pounds of unwanted body fat drinking delicious smoothies.
The signs of cardiac overload may be subtle at first, but recognizing them early and addressing the root cause—obesity—can lead to better outcomes.
The solution lies in early intervention, lifestyle changes, and medical management to reduce the heart’s workload and improve overall health.
References: