When it comes to heart health, HDL cholesterol is the golden child—often referred to as the “good cholesterol” for good reason.
It acts as a scavenger, collecting excess cholesterol from the bloodstream and transporting it back to the liver for disposal.
This process helps keep arteries clean and reduces the risk of heart disease.
But here is where the plot thickens: obesity, especially the stubborn kind that clings to your belly like a stage-five clinger, can sabotage HDL’s life-saving mission.
We are not just talking about weight on the scale—this is about visceral fat that wraps itself around internal organs and disrupts crucial metabolic functions.
Obesity does not just lower HDL levels; it also affects how HDL behaves. From increasing triglycerides to promoting chronic inflammation, excess fat throws HDL into a dysfunctional spiral.
The good guy turns less effective, losing its power to protect your arteries and combat cardiovascular disease.
This is far more serious than a lab report with slightly skewed numbers. It is a sign that your body’s cholesterol management system is breaking down.
In this article, the LeanAndFit research staff dives deep into how obesity drags HDL cholesterol down with it—and why this metabolic mess is a bigger deal than you might think.
Points Covered in this Article
- How Central Fat Silences HDL’s Party Tunes
- Adipose Tissue: The HDL Thief in the Biochemical Night
- Enzymatic Blockades: The HDL Metabolism Traffic Jam
- Inflammation, Insulin Resistance, and the HDL Domino Effect
- Altered HDL Quality: It’s Not Just the Quantity, It’s the Character
- Reverse Cholesterol Transport: When HDL Loses Driving Privileges
- FAQs on Obesity and Decreased HDL Cholesterol
- Weight Loss: The Comeback Tour for HDL
How Central Fat Silences HDL’s Party Tunes?
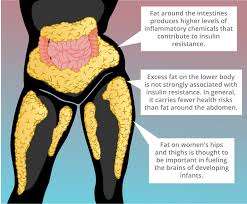
Let’s start with the obvious: belly fat is not just about squeezing into your jeans or blaming last night’s pizza.
Visceral fat—the deep, sneaky kind that hugs your organs from the inside—is far more dangerous than the stuff you can pinch.
It behaves less like passive storage and more like a hyperactive biochemical factory.
And one of its favorite pastimes? Ruining HDL cholesterol’s ability to function properly.
HDL, often dubbed the “good” cholesterol, is essential for mopping up excess cholesterol and ferrying it back to the liver.
But visceral fat throws a wrench into this life-saving routine. It floods your system with free fatty acids, cytokines and pro-inflammatory agents, which collectively impair the liver’s ability to produce and maintain healthy HDL levels.
That is like trying to throw a party while someone keeps unplugging the speakers—HDL never gets a chance to shine.
Even more mischievously, belly fat drives up triglyceride levels.
This activates a protein called CETP (cholesteryl ester transfer protein), which initiates a lipid trade that cheats HDL of its protective core. HDL ends up small, weak, and ineffective.
Think of it as losing the bouncers at a club—you still have a door, but anyone can walk in and wreck the vibe.
And here’s the kicker: even people with a “normal” BMI can have high visceral fat. Waist circumference matters more than you think.
A muffin top is not just cosmetic—it is often a silent saboteur of your HDL cholesterol.
So the next time your belt feels tight, consider it more than a wardrobe alert—it might be your body’s way of warning you about your heart health.
Adipose Tissue: The HDL Thief in the Biochemical Night
When fat cells multiply and expand, they do not just sit quietly. In obesity, adipose tissue turns into a chemically active monster that hijacks HDL particles.
Normally, HDL is built using components like cholesterol and a protein called apoA-I. But in obese individuals, fat cells hoard these raw materials, leaving less for HDL formation.
To make matters worse, the transporters responsible for moving cholesterol out of cells—ABCA1 and SR-BI—become sluggish.
So even if your body wants to make HDL, it’s working with limited ingredients and a broken conveyor belt.
The result? Less HDL is made, and what does get built is weak and ineffective.
Essentially, your fat cells are pulling off a stealthy cholesterol heist, robbing your body of the good guys.
Enzymatic Blockades: The HDL Metabolism Traffic Jam
Imagine HDL metabolism as a bustling freeway. In a lean body, traffic moves smoothly: HDL particles are formed, matured, and recycled with efficiency.
But with obesity, this freeway turns into a gridlock. One big reason is the enzyme CETP (cholesteryl ester transfer protein), which becomes overactive in obese individuals.
CETP swaps out HDL’s healthy contents for triglycerides, weakening its structure. Another culprit is hepatic lipase, which trims HDL particles down to a less functional size.
And as if that were not enough, the breakdown of apoA-I—the protein backbone of HDL—speeds up too.
All these factors shrink HDL, shorten its lifespan, and compromise its function.
It is like taking a luxury car and turning it into a rusty hatchback: it still moves, but not impressively.
Inflammation, Insulin Resistance, and the HDL Domino Effect
Obesity is not just about extra calories—it is about chronic and low-grade inflammation. Fat tissue in obese individuals releases pro-inflammatory cytokines like TNF-alpha and IL-6.
These inflammatory agents do not just cause aches and pains; they mess with cholesterol transporters, reducing HDL formation.
At the same time, this inflammation promotes insulin resistance, a condition where cells ignore insulin’s call. As insulin resistance builds, free fatty acids flood the bloodstream, pushing the liver to pump out more VLDL particles—fat carriers that compete with HDL.
VLDL essentially bullies HDL out of the spotlight, taking up enzymes and particles that HDL needs to survive.
The net result?
A downward spiral where inflammation and jeopardized glucose metabolism tag-team HDL into oblivion. It is a biochemical domino effect, and HDL is the last one standing—and falling.
Altered HDL Quality: It is Not Just the Quantity, It is the Character
If you think of HDL as the “good guy,” obesity doesn’t just reduce his numbers—it corrupts his personality.
In lean individuals, HDL particles are large, buoyant, and packed with antioxidant and anti-inflammatory power. But in people with obesity, HDL becomes small, dense, and dysfunctional.
It is still technically HDL, but it cannot do its job properly. These altered particles are poor at picking up cholesterol and are less protective for blood vessels.
Even worse, they can become pro-inflammatory under stress—meaning they may join the dark side.
So when doctors measure HDL cholesterol in obese patients, the number might look okay, but the particles themselves may be metabolically broken.
This proves once again: quality matters just as much—if not more—than quantity.
Reverse Cholesterol Transport: When HDL Loses Driving Privileges?
One of HDL’s most important roles is reverse cholesterol transport—essentially shuttling excess cholesterol from the arteries back to the liver for disposal.
In a healthy system, this is a smooth ride. But with obesity, the engine sputters. Cholesterol transporters like ABCA1 and ABCG1 become less active due to inflammation and insulin resistance. As a result, HDL can’t gather cholesterol efficiently.
Add in the excessive CETP activity, and whatever cholesterol HDL does collect often ends up being redirected to LDL and VLDL instead of the liver.
This is the molecular equivalent of HDL losing its driver’s license. The cholesterol builds up in arteries, increasing the risk of cardiovascular diseases such as high blood pressure.
So even if HDL is present, its ability to do its job—clear the roads of cholesterol traffic—is seriously compromised.
FAQs on Obesity and Decreased HDL Cholesterol:
Q-1: How does obesity lower HDL cholesterol levels in adults?
A: Obesity lowers HDL (good) cholesterol by disrupting lipid metabolism and increasing insulin resistance.
Excess body fat, especially visceral fat, alters how the body processes fats, leading to reduced HDL production and faster clearance from the bloodstream.
In the United States, over 42% of adults are classified as obese, and studies show a strong correlation between higher body fat and lower HDL levels.
This imbalance increases cardiovascular risk, as HDL plays a key role in removing excess cholesterol from arteries.
Q-2: What is the link between obesity and decreased HDL cholesterol risk factors in the USA?
A: The link between obesity and decreased HDL cholesterol involves multiple risk factors, including poor diet, inactivity, and metabolic dysfunction.
According to U.S. health data, approximately 13.8% of adults have low HDL cholesterol, with higher rates among overweight individuals.
Obesity amplifies these risks by increasing triglycerides and reducing HDL, creating a lipid profile associated with heart disease and stroke.
Q-3: Why is low HDL cholesterol common in overweight and obese individuals?
A: Low HDL cholesterol is common in overweight individuals because excess fat interferes with normal lipid transport and enzyme activity.
In the United States, about 74% of adults are overweight or obese, contributing to widespread lipid imbalances.
Increased fat mass leads to higher levels of triglycerides, which inversely affect HDL levels, resulting in reduced “good cholesterol” in circulation.
Q-4: Does belly fat reduce HDL cholesterol and increase heart disease risk?
A: Yes, belly fat significantly reduces HDL cholesterol and increases heart disease risk.
Abdominal obesity is strongly linked to metabolic syndrome, a condition affecting nearly 34% of U.S. adults.
Visceral fat releases inflammatory substances that lower HDL and promote plaque buildup in arteries, raising the likelihood of cardiovascular events such as heart attacks and strokes.
Q-5: What is the relationship between BMI and low HDL cholesterol levels?
A: There is a direct relationship between higher BMI and lower HDL cholesterol levels.
As BMI increases, HDL levels tend to decrease while triglycerides rise.
In the United States, individuals with a BMI over 30 are significantly more likely to have low HDL levels.
This relationship highlights the importance of maintaining a healthy weight to support optimal lipid balance and cardiovascular health.
Q-6: Can weight loss improve HDL cholesterol in obese adults naturally?
A: Yes, weight loss can naturally improve HDL cholesterol levels.
Losing even 5–10% of body weight has been shown to increase HDL levels and improve overall lipid profiles.
In U.S. clinical studies, individuals who achieved moderate weight loss experienced HDL increases of up to 10%.
This improvement reduces cardiovascular risk and enhances metabolic health.
Q-7: How does obesity cause atherogenic dyslipidemia and low HDL cholesterol?
A: Obesity contributes to atherogenic dyslipidemia, a condition characterized by low HDL, high triglycerides, and small dense LDL particles.
In the United States, this pattern is commonly observed in individuals with obesity and insulin resistance.
The condition accelerates plaque buildup in arteries, significantly increasing the risk of heart disease.
Q-8: What are the effects of obesity on HDL cholesterol and cardiovascular health in the USA?
A: Obesity negatively impacts HDL cholesterol and overall cardiovascular health by promoting inflammation, insulin resistance, and lipid imbalance.
In the United States, heart disease remains the leading cause of death, accounting for about 25% of all deaths.
Low HDL levels in obese individuals contribute to this risk by reducing the body’s ability to clear excess cholesterol from blood vessels.
Q-9: Why does obesity lead to low good cholesterol and high triglycerides?
A: Obesity leads to low HDL and high triglycerides due to impaired fat metabolism and increased fatty acid release from adipose tissue.
In the United States, this lipid pattern is seen in a significant portion of individuals with obesity.
Elevated triglycerides interfere with HDL formation, resulting in decreased levels of protective cholesterol.
Q-10: How does metabolic syndrome from obesity reduce HDL cholesterol levels?
A: Metabolic syndrome, often caused by obesity, reduces HDL cholesterol through a combination of insulin resistance, inflammation, and abnormal lipid processing.
In the United States, about 1 in 3 adults has metabolic syndrome, making it a major public health concern.
This condition lowers HDL levels while increasing cardiovascular risk, emphasizing the importance of early lifestyle interventions.
Weight Loss: The Comeback Tour for HDL
Now for some good news—HDL loves a comeback story. Studies consistently show that losing even a small percentage of body weight (around 5–10%) can significantly raise HDL levels.
This is especially true when the weight loss comes from reducing visceral fat.
Exercise—particularly aerobic workouts—boosts the enzymes that support HDL production and function.
Dietary changes help too, especially diets rich in monounsaturated fats like olive oil, nuts, and fatty fish.
Bariatric surgery has also been shown to restore HDL levels and improve particle quality.
The key takeaway?
HDL is resilient. Give it a better environment—less fat, fewer inflammatory signals, more physical movement—and it will rise again.
And this time, it comes back stronger, larger, and more functional, ready to reclaim its title as heart health’s MVP.
Bottom Line
Obesity and decreased HDL cholesterol are more than casual acquaintances—they are co-conspirators in undermining heart health.
From impaired HDL production and altered enzyme activity to chronic inflammation and disrupted cholesterol transport, obesity throws a wrench in nearly every part of HDL’s function. But this is not a hopeless story.
With targeted lifestyle changes—like weight loss, regular exercise, and smarter food choices—you can flip the script. HDL does not just return; it comes back better equipped to protect your heart, clean up excess cholesterol, and reduce inflammation.
So while a healthy weight might not be the flashiest goal, it is one that quietly rebuilds the very molecules keeping your heart safe.
And that, in any medical playbook, is a win worth celebrating.
References: