Obesity rates have surged across the american population, with over 42 percent of adults now meeting medical criteria for this chronic condition.
This widespread issue goes far beyond appearance or simple weight gain, affecting long-term health and daily life in profound ways.
Understanding how obesity is defined, its impact on major diseases, and the latest medical insights empowers individuals to make informed choices for better health outcomes.
Table of Contents
- Defining Obesity and Its Medical Criteria
- Major Chronic Diseases Linked to Obesity
- Metabolic and Hormonal Impacts of Obesity
- Mental and Social Consequences of Obesity
- Prevention and Management Strategies for Obesity
Key Takeaways
| Point | Details |
|---|---|
| Obesity Definition | Obesity is defined as excessive body fat that affects health, and recent criteria now include waist circumference and body fat distribution for a comprehensive assessment. |
| Chronic Disease Risks | Obesity is a major risk factor for diseases like cardiovascular issues, Type 2 diabetes, and certain cancers, necessitating proactive intervention strategies. |
| Metabolic Impacts | Obesity leads to hormonal and metabolic dysregulation, increasing the risk of chronic diseases and creating challenges in weight management. |
| Psychological Effects | The social stigma of obesity can lead to mental health issues, including depression and anxiety, underscoring the need for supportive interventions. |
Defining Obesity and Its Medical Criteria
Obesity is a complex medical condition characterized by excessive body fat accumulation that significantly impacts an individual’s overall health. Unlike simple weight gain, obesity represents a chronic metabolic disorder with specific medical diagnostic criteria.
The traditional method of defining obesity has primarily relied on Body Mass Index (BMI), a calculation based on an individual’s height and weight.
Recently, medical researchers have proposed a more nuanced approach to obesity diagnosis. According to the Lancet Commission, the definition of clinical obesity now integrates BMI with additional anthropometric measurements, such as waist circumference.
This comprehensive method provides a more accurate assessment of health risks associated with excess body fat. By considering body fat distribution beyond a single numerical metric, healthcare professionals can better identify individuals at potential metabolic risk.
The updated diagnostic criteria reveal significant insights into obesity prevalence. Mass General Brigham researchers observed a substantial increase in obesity rates when applying these expanded diagnostic standards.
The new definition considers several key factors:
- Waist circumference measurements
- Total body fat percentage
- Fat distribution patterns
- Metabolic health indicators
These refined criteria acknowledge that obesity is not merely about weight, but about complex metabolic interactions that influence overall health risk.
Understanding these nuanced medical standards is crucial for individuals seeking comprehensive health assessments and potential intervention strategies.
Major Chronic Diseases Linked to Obesity
Obesity represents a significant public health challenge, acting as a critical risk factor for numerous chronic diseases that can dramatically reduce quality of life and life expectancy.
National Center for Biotechnology Information research highlights obesity as a key modifiable risk factor for multiple severe health conditions, emphasizing the critical need for comprehensive prevention and management strategies.
Cardiovascular diseases emerge as one of the most prominent health risks associated with obesity.
Houston Methodist Journal researchers note that obesity triggers intricate metabolic and biochemical dysfunctions that significantly increase the likelihood of heart disease, hypertension, and related cardiovascular complications.
The excess body fat contributes to inflammation, insulin resistance, and abnormal lipid profiles, which directly compromise heart and blood vessel health.
Beyond cardiovascular concerns, obesity substantially elevates risks for several chronic conditions:
- Type 2 Diabetes Mellitus
- Certain Cancers
- Metabolic Syndrome
- Respiratory Disorders
- Reproductive Health Issues
These chronic diseases are interconnected, often creating complex health challenges that extend far beyond simple weight management.
 Understanding these risks underscores the importance of proactive lifestyle interventions and comprehensive medical approaches to addressing obesity and its potential long-term health consequences.
Understanding these risks underscores the importance of proactive lifestyle interventions and comprehensive medical approaches to addressing obesity and its potential long-term health consequences.
Metabolic and Hormonal Impacts of Obesity
Metabolic dysregulation represents a complex cascade of biological changes triggered by obesity, fundamentally altering the body’s core physiological processes.
National Center for Biotechnology Information research reveals that obesity influences multiple critical systems, including genetic, neurologic, metabolic, and behavioral mechanisms, creating a profound disruption of normal bodily functions.
Houston Methodist Journal researchers have extensively documented the intricate hormonal changes associated with obesity. These metabolic alterations extend far beyond simple weight gain, profoundly impacting the body’s hormonal balance.
Key hormonal disruptions include:
- Insulin resistance
- Altered adipokine secretion
- Increased inflammatory markers
- Disrupted leptin and ghrelin signaling
- Compromised cortisol regulation
The interconnected nature of these metabolic and hormonal changes creates a complex physiological environment that can significantly increase risks of chronic diseases.
Excess body fat acts as an active endocrine organ, continuously releasing hormones and inflammatory compounds that fundamentally reshape metabolic functioning.
These disruptions can trigger a self-perpetuating cycle of metabolic dysfunction, making weight management increasingly challenging for individuals struggling with obesity.
Mental and Social Consequences of Obesity
Social stigma surrounding obesity represents a profound psychological challenge that extends far beyond physical health implications.
Houston Methodist Journal research reveals that obesity is deeply linked to significant psychosocial dysfunctions, including depression and social marginalization that can severely impact an individual’s mental well-being and overall quality of life.
Mass General Brigham researchers highlight how evolving societal perceptions can intensify psychological challenges. The expanded definitions of obesity potentially amplify mental health risks by reshaping social interactions and self-perception.
Key mental and social consequences include:
- Increased risk of depression
- Higher likelihood of social anxiety
- Reduced self-esteem
- Workplace discrimination
- Potential social isolation
These psychological impacts create a complex emotional landscape where individuals with obesity often experience a cyclical pattern of stress, social withdrawal, and diminished mental resilience.
The internalized stigma can lead to profound emotional suffering, potentially exacerbating existing health challenges and creating additional barriers to successful weight management and personal well-being.
Prevention and Management Strategies for Obesity
Comprehensive obesity management requires a multifaceted approach that addresses the complex physiological and behavioral factors contributing to weight gain.
National Center for Biotechnology Information research highlights the importance of individualized treatment plans that incorporate various intervention strategies tailored to each person’s unique health profile.
Houston Methodist Journal experts emphasize that addressing obesity demands a holistic approach combining multiple treatment modalities.
The primary strategies for prevention and management include:
- Personalized dietary interventions
- Regular physical activity programs
- Behavioral therapy and psychological support
- Medical treatments and pharmacotherapies
- Potential surgical interventions for severe cases
Successful obesity management is not about a one-size-fits-all solution, but rather a dynamic, personalized approach that adapts to an individual’s specific health needs, metabolic challenges, and lifestyle constraints.
By integrating medical, nutritional, psychological, and lifestyle interventions, individuals can develop sustainable strategies for weight management and overall health improvement.
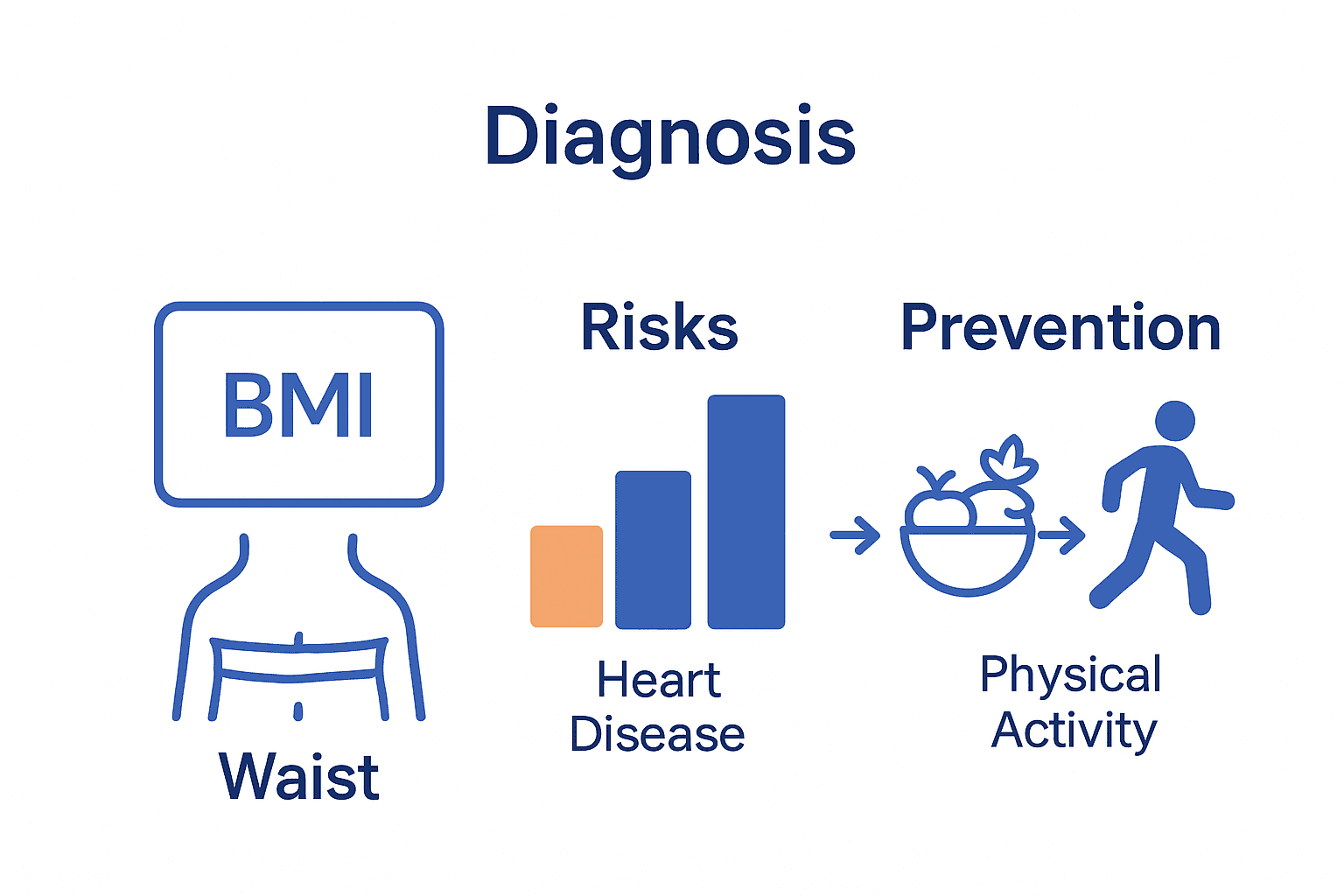
Take Control of Your Health by Understanding Obesity and Its Risks
Obesity is more than just a number on the scale.
This article highlights the serious challenges of metabolic and hormonal imbalances, increased risks of heart disease, and conditions like insulin resistance that deeply affect your well-being.
If you are struggling with managing your weight or worried about the hidden health risks linked to obesity, you are not alone.
Understanding these complex effects is the first step toward lasting change.
At LeanAndFit you will find trusted resources tailored to help you fight obesity through proven natural methods including effective lifestyle changes, personalized dietary plans, and supportive fitness routines aimed at improving your metabolic health.
Do not wait until obesity-related health issues worsen.
Discover how to protect your heart, regulate blood sugar, and rebuild your confidence. Start transforming your health today by visiting LeanAndFit and take the empowered path to a fitter future.
Frequently Asked Questions
Q-1: How does obesity impact brain health?
A-1: Obesity, especially excess fat around the abdomen, is linked to a reduction in grey matter in the brain. This can impair cognitive abilities and increase the risk of neurodegenerative diseases. Chronic inflammation from obesity is believed to play a significant role in these negative brain effects.
Q-2: What is the relationship between obesity and organ size?
A-2: Obesity causes enlargement of certain organs such as the liver, kidneys, and pancreas. Larger organ size means more cells are present, which increases the likelihood of cellular abnormalities and raises the risk of developing cancers in these organs.
Q-3: How does obesity affect life expectancy?
A-3: Severe obesity can reduce life expectancy by up to 14 years compared to individuals with a healthy weight. This decrease is largely due to obesity-related illnesses like cardiovascular disease, stroke, and diabetes.
Q-4: What are the economic implications of obesity?
A-4: Obesity creates a significant financial strain on healthcare systems due to the high costs of treating related diseases. Beyond medical expenses, obesity also leads to productivity losses caused by absenteeism and decreased work performance.
Q-5: How does obesity influence sleep quality?
A-5: Obesity increases the risk of obstructive sleep apnea, a disorder where breathing repeatedly stops during sleep. This condition disrupts restful sleep, causes daytime fatigue, and elevates the risk for heart problems.
Q-6: What is the impact of obesity on mental health?
A-6: Obesity is associated with increased rates of depression, anxiety, and lowered self-esteem. Physical limitations and social stigma connected to obesity often contribute to these mental health challenges.
Q-7: How does obesity affect reproductive health?
A-7: Obesity can cause menstrual irregularities, infertility, and complications during pregnancy. Women with obesity are more likely to develop conditions such as polycystic ovary syndrome (PCOS), which can impair fertility and reproductive function.